Is There a Vaccine Coming?
When will there be a Vaccine?
There are vaccines being developed and some should be ready with weeks or even days for small clinical trials. The problem is that once developed and showed helpful, it will take a year to 18 months to determine if it is safe, effective and to confirm dosage levels. The vaccine would have to pass tests and be approved by the National Institute of Allergy and Infectious Diseases (led for many years by Dr. Anthony Fauci) which is part of the National Institutes of Health (NIH).
Luckily, Dr. Fauci despite his advanced age, continues to use his many years of experience to fight these new coronaviruses. His long-term leadership and straight-forward, honest style has help induce some confidence in an otherwise scary scenario. Another person to listen to is Dr. Nancy Messonnier, director of the CDC’s National Center for Immunization and respiratory Diseases.
The first vaccine was developed for flu in the 1940s, which inserts some flu material (dead virus) into you so you can develop antibodies in advance to fight off the infection before it takes hold. You can see the importance of this in novel diseases, where no one has previous immunity.
Small pox vaccines were originally made from serum taken from milkmaids who developed a benign, but disfiguring, disease called cowpox on their hands from milking cows. A British man, Dr. Edward Jenner, noticed milkmaids seemed immune to smallpox. He had the idea that injecting matter from cowpox pustules into people might help them develop immunity (antibodies) to the similar smallpox virus to allow them to fight off the disease (causing immunity) before they could be severely sickened. Below is a painting depicting Dr. Edward Jenner performing the first known smallpox vaccination. It wouldn’t hold up to today’s HIPAA standards, as he injected his gardiner’s 9-year-old grandson and then exposed the boy to smallpox in order to test his vaccination idea. Luckily it worked.
There are vaccines being developed and some should be ready with weeks or even days for small clinical trials. The problem is that once developed and showed helpful, it will take a year to 18 months to determine if it is safe, effective and to confirm dosage levels. The vaccine would have to pass tests and be approved by the National Institute of Allergy and Infectious Diseases (led for many years by Dr. Anthony Fauci) which is part of the National Institutes of Health (NIH).
Luckily, Dr. Fauci despite his advanced age, continues to use his many years of experience to fight these new coronaviruses. His long-term leadership and straight-forward, honest style has help induce some confidence in an otherwise scary scenario. Another person to listen to is Dr. Nancy Messonnier, director of the CDC’s National Center for Immunization and respiratory Diseases.
The first vaccine was developed for flu in the 1940s, which inserts some flu material (dead virus) into you so you can develop antibodies in advance to fight off the infection before it takes hold. You can see the importance of this in novel diseases, where no one has previous immunity.
Small pox vaccines were originally made from serum taken from milkmaids who developed a benign, but disfiguring, disease called cowpox on their hands from milking cows. A British man, Dr. Edward Jenner, noticed milkmaids seemed immune to smallpox. He had the idea that injecting matter from cowpox pustules into people might help them develop immunity (antibodies) to the similar smallpox virus to allow them to fight off the disease (causing immunity) before they could be severely sickened. Below is a painting depicting Dr. Edward Jenner performing the first known smallpox vaccination. It wouldn’t hold up to today’s HIPAA standards, as he injected his gardiner’s 9-year-old grandson and then exposed the boy to smallpox in order to test his vaccination idea. Luckily it worked.
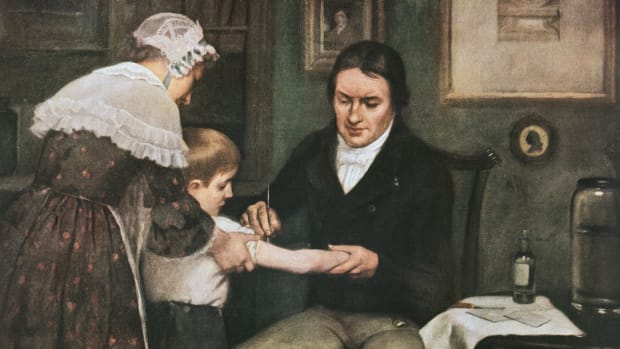
Remember we talked about the issue with “novel” viral infections? The problem being few people had survived a new disease in order to develop immunity. Once enough people develop immunity, an epidemic is hard to start since crowded conditions lead to less spread if a certain percentage of people have immunity; this is called the “herd effect.” When small pox arrived in the America’s in the 15th century with Spanish explorers the native people of modern-day US and Mexico had no natural immunity and they died by the tens of millions (90 to 95% of the population) to Small Pox.
Are there Treatments Once you Contract COVID-19?
At the moment treatments are limited to supportive care, to give the patient’s own immune system time to fight off the infection. For serious respiratory illness the most important component of such care are the ventilators you read about in the news. These are are expensive (around $20–25,000) and we have far too few in hospitals, nursing homes and in military settings for the numbers of patients likely to develop inability to breath without them. Hospitals are already considering rationing as to who to put on ventilators and who not to. They may limit people to around 120 hours on them and terminate the treatment if no improvement is seen. Again, this affects seniors more than other populations, as well as anyone with asthma or lung problems. Without good treatment options available, should you develop severe illness the odds decline with your age and health status. Your best treatment is to not get infected in the first place, and adhere to social distancing and self-isolation as much as possible.
Gene sequencing of the virus allows us to see similarities to other disease where treatments have been effective. One encouraging sign is that there are a number of drugs already approved for treatment of other coronavirus caused diseases like Ebola and SARS which might prove helpful in treating COVID-19 patients.
Disinfecting
Please refer to the previous section for information about disinfecting surfaces and cleaning regarding how to kill all coronaviruses. Don’t forget your cell phone!
Good Habits to Develop
Oddly, it’s not so much avoiding people that works to protect yourself. Keeping six feet away usually solves that problem. Rather, it’s how you interact with things like door knobs and then touching your face that will most likely to lead to infection. Other than breathing in droplets from others, the most common means to spread the virus is from touching surfaces and then touching your face. What you touch can be transferred when you touch your eyes and other mucous membranes, which is how we typically acquire respiratory infections. Yes washing your hands is very important. But, sanitizing surfaces you are likely to come in contact before and after you wash is also critical to avoid giving/getting the virus.
Coronaviruses can live on hard surfaces for hours to days. We’re still learning about COVID-19, but we can assume it will live on surfaces for two–20 hours, so keep sanitizer wipes (hard to get them just now) in the car to wipe down door handles, the steering wheel, shift knob, etc.